In post hoc and real-world analyses, SARCLISA-based regimens demonstrated efficacy1,2
Across cytogenetic risk profiles
Regardless of early or late relapse
Regardless of the number of prior lines of therapy
Cytogenetic Risk Profiles
SUBGROUP ANALYSIS OF THE IKEMA TRIAL
SARCLISA + Kd demonstrated 42.4 months mPFS in the standard-risk subgroup and nearly doubled ≥CR and MRD- in standard-risk and extended high-risk subgroups1
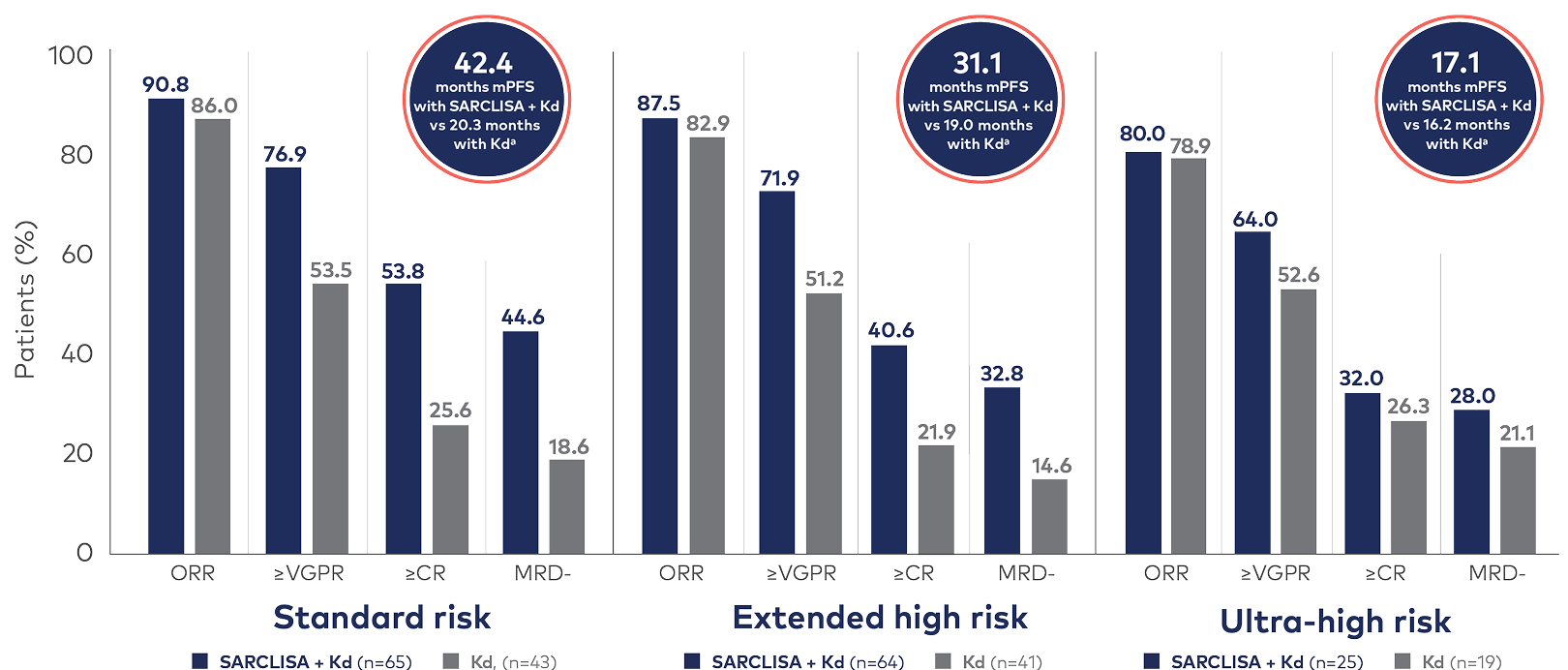
Adapted from Moreau et al. Presented at: European Hematology Association (EHA) 2023 Hybrid Congress; June 8-11, 2023; Frankfurt, Germany and online. See original graphics in Moreau et al. (Figure 5 and Figure 6).
- Standard risk was defined as the absence of the following high-risk cytogenetic abnormalities: del(17p), t(4;14), t(14;16), and 1q21+, which included both gain(1q21) and amp(1q21)1
- Extended high risk was defined as the presence of 1 of these high-risk cytogenetic abnormalities1
- Ultra-high risk was defined as the presence of ≥2 high-risk cytogenetic abnormalities1
mPFS was measured for different subgroups, including standard-risk at 42.4 months (HR=0.496 [95% Cl: 0.294, 0.839]), extended high-risk at 31.1 months (HR=0.531 [95% Cl: 0.310, 0.908]), and ultra-high-risk at 17.1 months (HR=0.689 [95% Cl: 0.343, 1.385]).1
At the time of data cutoff, the OS data were immature. Trial analysis is ongoing.1
Key takeaway
Regardless of cytogenetic risk, SARCLISA + Kd is associated with extended PRFS, deeper responses, and increased rates of MRD- vs Kd alone
For more information about the phase 3 IKEMA study, view SARCLISA + Kd trial design.
Early and late relapse
POST HOC SUBGROUP ANALYSIS OF THE IKEMA TRIAL
Median PFS was 20.8 months longer in late relapse with SARCLISA + Kd vs Kd alone2
Late Relapse
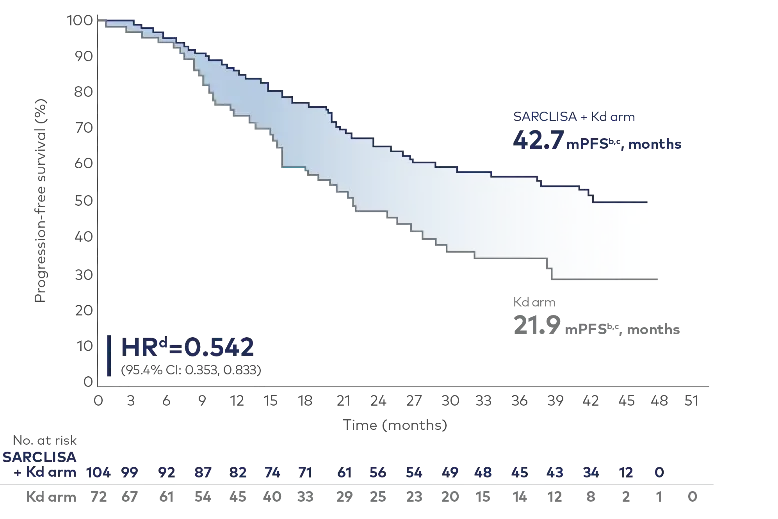
Cut-off date: January 14, 2022. Median follow-up time: 44 months.2
Median PFS was 7.5 months longer in early relapse with SARCLISA + Kd vs Kd alone2
EARLY RELAPSE
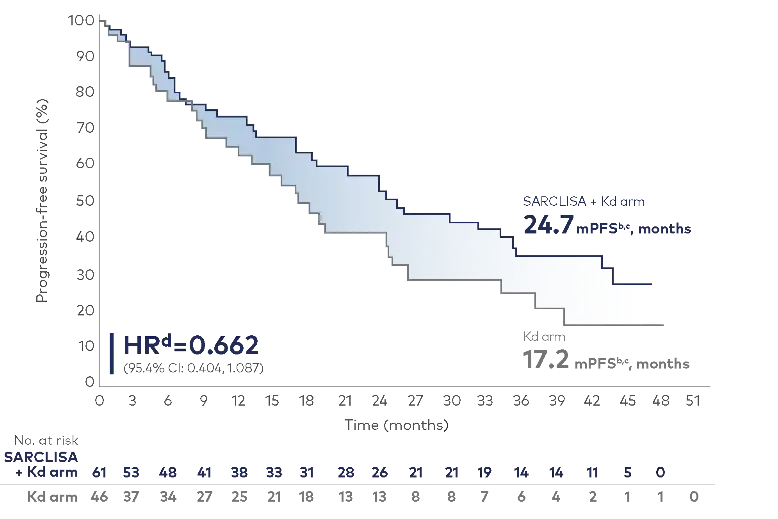
Cut-off date: January 14, 2022. Median follow-up time: 44 months.2
Early and late relapse definitions2
Early relapse* (n=107 [n=61, SARCLISA + Kd; n=46, Kd alone])
- Relapsed <12 months from initiation of the most recent line of therapy for patients with ≥2 prior lines of therapy
- Relapsed <18 months for patients with 1 prior line of therapy
- Relapsed <12 months from ASCT
Late relapse* (n=176 [n=104, SARCLISA + Kd; n=72, Kd alone])
- Relapsed ≥12 months from initiation of the most recent line of therapy for patients with ≥2 prior lines of therapy
- Relapsed ≥18 months for patients with 1 prior line of therapy
Depth of response was higher in both early and late relapse patients with rates of MRD- and MRD- ≥CR nearly doubled in SARCLISA + Kd vs Kd alone2
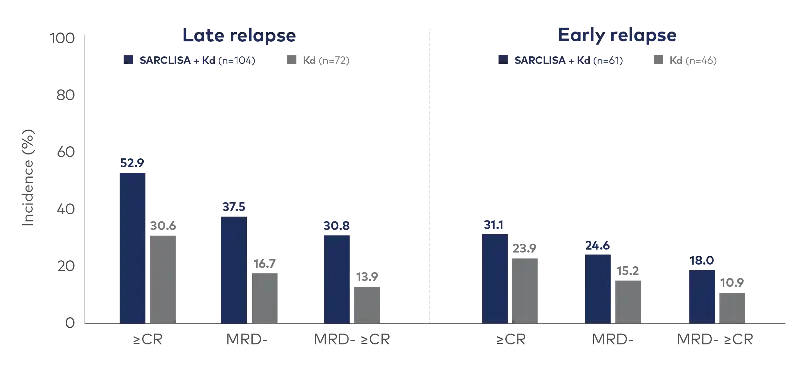
Adapted from Facon et al. Presented at: 64th ASH (American Society of Hematology) Annual Meeting and Exposition; December 10-13, 2022; New Orleans, Louisiana. See original graphics in Facon et al. (page 11).
Cut-off date: January 14, 2022. Median follow-up time: 44 months.2
MRD- was assessed by next-generation sequencing with the adaptive clonoSEQ® assay (Adaptive Biotechnologies Corporation) at 10-5 sensitivity.2
For analysis purpose, patients in the ITT population but without MRD assessment were considered to have possible MRD.2
clonoSEQ is a registered trademark of Adaptive Biotechnologies Corp.
Key takeaway
Notable efficacy in early relapse patients and robust efficacy in late relapse patients supports SARCLISA + Kd as a standard of care for both subgroups2
IKEMA Safety Profile1
SARCLISA + Kd was well tolerated across all risk category subgroups in the phase 3 IKEMA trial. The incidence of Grade ≥3 treatment-emergent adverse events was generally higher in the SARCLISA + Kd arm than the control arm, regardless of risk profile, with the exception of standard-risk patients.1
In the IKEMA dataset, for standard-risk patients, the most frequent Grade ≥3 TEAEs and haematologic abnormalities were neutropenia (15.4%), thrombocytopenia (21.5%), hypertension (24.6%), anaemia (16.9%), pneumonia (16.9%), and cardiac failure (1.5%), with no reported infusion-related reactions. Extended high-risk patients showed neutropenia (17.5%), thrombocytopenia (33.3%), anaemia (33.3%), pneumonia (17.5%), and hypertension (25.4%), with no infusion-related reactions but some cardiac failure (4.8%). Ultra-high-risk patients experienced neutropenia (40.0%), thrombocytopenia (32.0%), anaemia (28.0%), pneumonia (28.0%), hypertension (20.0%), and some infusion-related reactions (4.0%), with no cardiac failure reported.1
In the IKEMA dataset, for late relapse patients, the most frequent ≥3 TEAEs and Grade 3 haematologic abnormalities were hypertension (21.6%), pneumonia (18.6%), thrombocytopenia (16.7%), anaemia (13.7%), neutropenia (13.7%), dyspnoea (7.8%), fatigue (6.9%), bronchitis (2.9%), diarrhoea (2.9%), upper respiratory tract infection (2.9%), cardiac failure (2.0%), and infusion reaction (1.0%).2
In the IKEMA dataset, for early relapse patients, the most frequent ≥3 TEAEs and Grade 3 haematologic abnormalities were anaemia (42.6%), thrombocytopenia (21.3%), hypertension (19.7%), neutropenia (18.0%), pneumonia (18.0%), fatigue (4.9%), cardiac failure (3.3%), diarrhoea (3.3%), dyspnoea (3.3%), gastroenteritis (3.3%), and upper respiratory tract infection (3.3%).2
aThe 95% confidence interval for standard risk, extended high risk, and ultra-high risk were (0.294, 0.839), (0.310, 0.908), and (0.343, 1.385), respectively.1
bAs per IRC.2
cMedian PFS and Cls were calculated by the Kaplan-Meier method.2
dUnstratified HR estimates were determined using the non-stratified Cox proportional hazard model using treatment as covariate. Adjusted HR estimates were determined after adjusting for confounding factors (age, renal impairment, ISS stage at study entry, 1q21+, and number of prior lines). When adjusted for confounding factors, the PFS HR was similar between early (0.577) and late relapse (0.527) patients.2
*Includes relapsed and refractory MM (excludes primary refractory).2
ASCT=autologous stem cell treatment; CR=complete response; HR=hazard ratio; IRC=Independent Review Committee; ISS=International Staging System; ITT=intent to treat; Kd=carfilzomib and dexamethasone; mPFS=median progression-free survival; MRD=minimal residual disease; MRD-=minimal residual disease negative/negativity; ORR=overall response rate; OS=overall survival; Pd=pomalidomide and dexamethasone; PFS=progression free survival; RRMM=relapsed and/or refractory multiple myeloma; TEAE=treatment-emergent adverse event; VGPR=very good partial response.
References: 1. Moreau P, Perrot A, Dimopoulos MA, et al. Isatuximab in relapsed multiple myeloma patients with ultra-high-risk cytogenetics: ICARIA-MM and IKEMA subgroup analysis. Poster presented at: European Hematology Association (EHA) 2023 Hybrid Congress; June 8-11, 2023; Frankfurt, Germany and online. 2. Facon T, Moreau P, Baker R, et al. Isatuximab plus carfilzomib and dexamethasone in pts with early versus late relapsed multiple myeloma: IKEMA subgroup analysis. Presented at: 64th ASH Annual Meeting and Exposition; December 10-13, 2022; New Orleans, LA. ID #753. doi:10.1111/ejh.14225
Sanofi does not recommend the use of its products in any manner inconsistent with that described in the label available in your country. Please refer to your local product labelling information before prescribing.
Name and Presentation: SARCLISA 20 mg/mL concentrate for solution for infusion. Each vial contains 100 mg of isatuximab in 5 mL of concentrate (100 mg/5 mL) or 500 mg of isatuximab in 25 mL of concentrate (500 mg/25 mL). Isatuximab is an immunoglobulin G1 (IgG1) monoclonal antibody (mAb).
Therapeutic indications: In combination with pomalidomide and dexamethasone, for the treatment of adult patients with relapsed and refractory multiple myeloma (MM) who have received at least two prior therapies including lenalidomide and a proteasome inhibitor (PI) and have demonstrated disease progression on the last therapy. In combination with carfilzomib and dexamethasone, for the treatment of adult patients with multiple myeloma who have received at least one prior therapy. In combination with bortezomib, lenalidomide, and dexamethasone, for the treatment of adult patients with newly diagnosed multiple myeloma who are ineligible for autologous stem cell transplant.
Pediatric population: Outside its authorised indications, SARCLISA has been studied in children aged 28 days to less than 18 years of age with relapsed or refractory acute lymphoblastic or myeloid leukaemia but efficacy has not been established.
Dosage and administration: SARCLISA should be administered by a healthcare professional, in an environment where resuscitation facilities are available. Premedication should be used 15-60 minutes prior to SARCLISA infusion with the following medicinal products to reduce the risk and severity of infusion reactions: Dexamethasone 40 mg (when administered in combination with isatuximab and pomalidomide) or 20 mg (when administered in combination with isatuximab and carfilzomib; or when administered in combination with isatuximab, bortezomib, and lenalidomide) oral or intravenous, 20 mg for patients ≥75 years of age, Acetaminophen, Diphenhydramine, H2 antagonists. The recommended dose of SARCLISA is 10 mg/kg body weight administered as an intravenous infusion in combination with pomalidomide and dexamethasone or in combination with carfilzomib and dexamethasone or in combination with bortezomib, lenalidomide, and dexamethasone (isatuximab regimen). Dosing schedule in combination with pomalidomide and dexamethasone or in combination with carfilzomib and dexamethasone: cycle 1: days 1, 8, 15 and 22 (weekly), cycle 2 and beyond: days 1, 15 (every 2 weeks). Each treatment cycle consists of a 28-day period. Dosing schedule in combination with bortezomib, lenalidomide, and dexamethasone: cycle 1: days 1, 8, 15, 22 and 29, cycles 2 to 4: days 1, 15 and 29 (every 2 weeks), cycles 5 to 17: days 1 and 15 (every 2 weeks), cycles 18 and beyond: day 1 (every 4 weeks). Each treatment cycle consists of a 42-day period from cycle 1 to 4, and of a 28-day period from cycle 5. Treatment is repeated until disease progression or unacceptable toxicity.
Method of administration: SARCLISA is for intravenous use. For details on preparation and infusion rate see full SmPC.
Contraindications: Hypersensitivity to the active substance or to any of the excipients. See full SmPC for full list of excipients.
Warnings and precautions: Infusion reactions, mostly mild or moderate, were observed in 38.2% of patients treated with SARCLISA in ICARIA, and in 45.8% in IKEMA but resolved on the same day in 98% of infusions, and in 24.0% of patients treated with Isa-VRd in IMROZ and resolved the same day in 97.3% of patients. The most common symptoms of an IR included dyspnoea and chills. The most common severe sign and symptom was hypertension. Vital signs should be frequently monitored during the entire infusion and when required infusion should be interrupted or permanently discontinued in case symptoms that do not improve to grade ≤1 after infusion interruption. Serious infusion reactions including severe anaphylactic reactions have also been observed after SARCLISA administration. Most of the grade 3-4 neutropenia was reported as laboratory abnormalities. In patients treated with Isa-VRd, neutropenia was reported as a laboratory abnormality in 87.5% of patients and as an adverse reaction in 30% of patients. Neutropenic complications have been observed in 1/3 of patients treated with SARCLISA. A higher incidence of infections including grade ≥3 infections occurred with SARCLISA. Antibacterial and antiviral prophylaxis (such as herpes zoster prophylaxis) according to treatment guidelines should be considered during treatment. Patients receiving SARCLISA should be closely monitored for signs of infection. Physicians should carefully evaluate patients before and during treatment as per International Myeloma Working Group (IMWG) guidelines for occurrence of secondary primary malignancies (SPM) and treatment should be initiated as indicated. Patients should be monitored closely, and appropriate precautions taken for tumor lysis syndrome. Isatuximab binds to CD38 on red blood cells (RBCs) and may result in a false positive indirect antiglobulin test (indirect Coombs test). This interference with the indirect Coombs test may persist for at least 6 months after the last infusion of SARCLISA. Patient should have blood type and screen tests performed prior to the first infusion of Isatuximab and should be monitored for theoretical risk of haemolysis. For details in tests interference see full SmPC.
Drug interactions: Isatuximab has no impact on the pharmacokinetics of pomalidomide or carfilzomib, or bortezomib, or lenalidomide and vice versa. Isatuximab may interfere with serological testing and with Serum Protein Electrophoresis and Immunofixation assays. In patients with persistent very good partial response, where isatuximab interference is suspected, consider using a validated isatuximab-specific IFE assay to distinguish isatuximab from any remaining endogenous M protein in the patient’s, to facilitate determination of complete response.
Fertility, pregnancy and lactation: Women of childbearing potential treated with isatuximab should use effective contraception during treatment and for 5 months after cessation of treatment. The use of isatuximab in pregnant women is not recommended since there are no available data.
Undesirable effects: Observed in patients treated with isatuximab in combination with pomalidomide and dexamethasone: Infections/infestations: very common: pneumonia, upper respiratory tract infection, bronchitis: common: Herpes zoster. Neoplasms benign, malignant and unspecified: common: skin cancer, solid tumour (non-skin cancer): uncommon: haematology malignancy. Blood/lymphatic system disorders: very common: neutropenia, thrombocytopenia, common: febrile neutropenia, anaemia, unknown frequency: lymphopenia. Metabolism and nutrition disorders: very common: decreased appetite. Cardiac disorders: common: atrial fibrillation. Respiratory, thoracic and mediastinal disorders: very common: dyspnoea. Gastrointestinal disorders: very common: diarrhoea, nausea, vomiting. Investigations: common: weight decreased. Injury, poisoning and procedural complications: very common: infusion reaction. Immune system disorders: uncommon: anaphylactic reaction. Observed in patients treated with isatuximab in combination with carfilzomib and dexamethasone: Infections/infestations: very common: pneumonia, upper respiratory tract infection, bronchitis: common: Herpes Zoster. Vascular disorder: very common: hypertension. Neoplasms benign, malignant and unspecified: common: Skin cancers and solid tumors non-skin cancers. Blood/lymphatic system disorders: common: neutropenia, anaemia, thrombocytopenia, unknown frequency: lymphopenia. Respiratory, thoracic and mediastinal disorders: very common: dyspnoea and cough. Gastrointestinal disorders: very common: diarrhoea and vomiting. General disorders and administration site conditions: very common: Fatigue. Injury, poisoning and procedural complications: very common: infusion reaction. Immune system disorders: uncommon: anaphylactic reaction. Reported in patients with multiple myeloma treated with isatuximab in combination with bortezomib, lenalidomide, and dexamethasone: Infections/infestations: very common: pneumonia, bronchitis, Covid-19. Neoplasms benign, malignant and unspecified: common: skin cancer, solid tumour, uncommon: haematology malignancy. Blood and lymphatic system disorders: very common: neutropenia, thrombocytopenia, common: anaemia, not known: lymphopenia. Immune system disorders: uncommon: anaphylactic reaction. Eye disorders: very common: cataract. Gastrointestinal disorders: very common: diarrhoea, common: vomiting. General disorders and administration site conditions: very common: fatigue. Injury, poisoning and procedural complications: very common: infusion reaction.
Pharmacotherapeutic group: Antineoplastic agents, monoclonal antibodies, ATC code: L01FC02.
List of excipients: Sucrose, Histidine hydrochloride monohydrate, Histidine, Polysorbate 80 and Water for injections.
Legal classification: Prescription Only Medicine.
Marketing authorization holder: Sanofi Winthrop Industrie, 82, avenue Raspail, 94250 Gentilly, France.
Date of last revised: March 2025.
Abbreviated Prescribing Information based on the EU SmPC as of February 2025.
Before prescribing always refer to your full local prescribing information as this information may vary from country to country
MAT-GLB-2101917-v10.0-03/2025
