- Article
- Source: Campus Sanofi
- 19 Dec 2025
The pathophysiology of ITP stems from complex immune dysregulation drives thrombocytopenia and inflammation
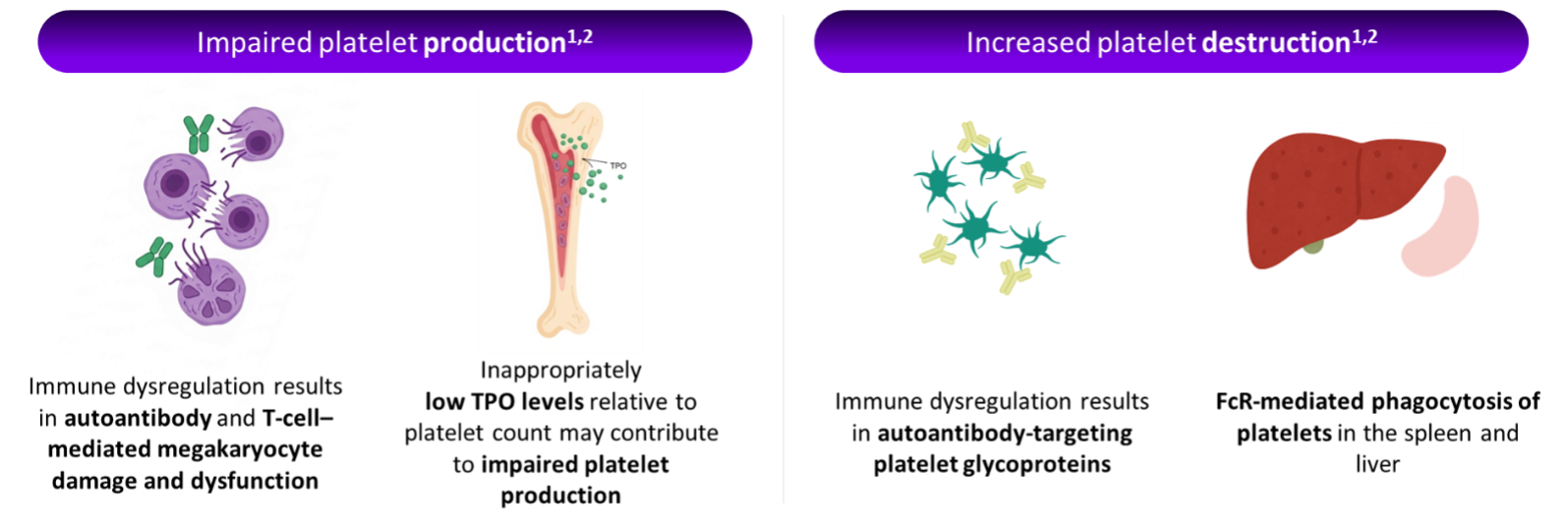
The pathophysiology of ITP stems from complex immune dysregulation leading to two primary mechanisms*
.2025-12-19-16-11-45.png)
The underlying cause of ITP is complex immune dysregulation that involves multiple components of the innate and adaptive immune system driving autoimmunity and systemic inflammation1,3,4
The pathophysiology of ITP stems from complex immune dysregulation drives thrombocytopenia and inflammation.1,2,5-12
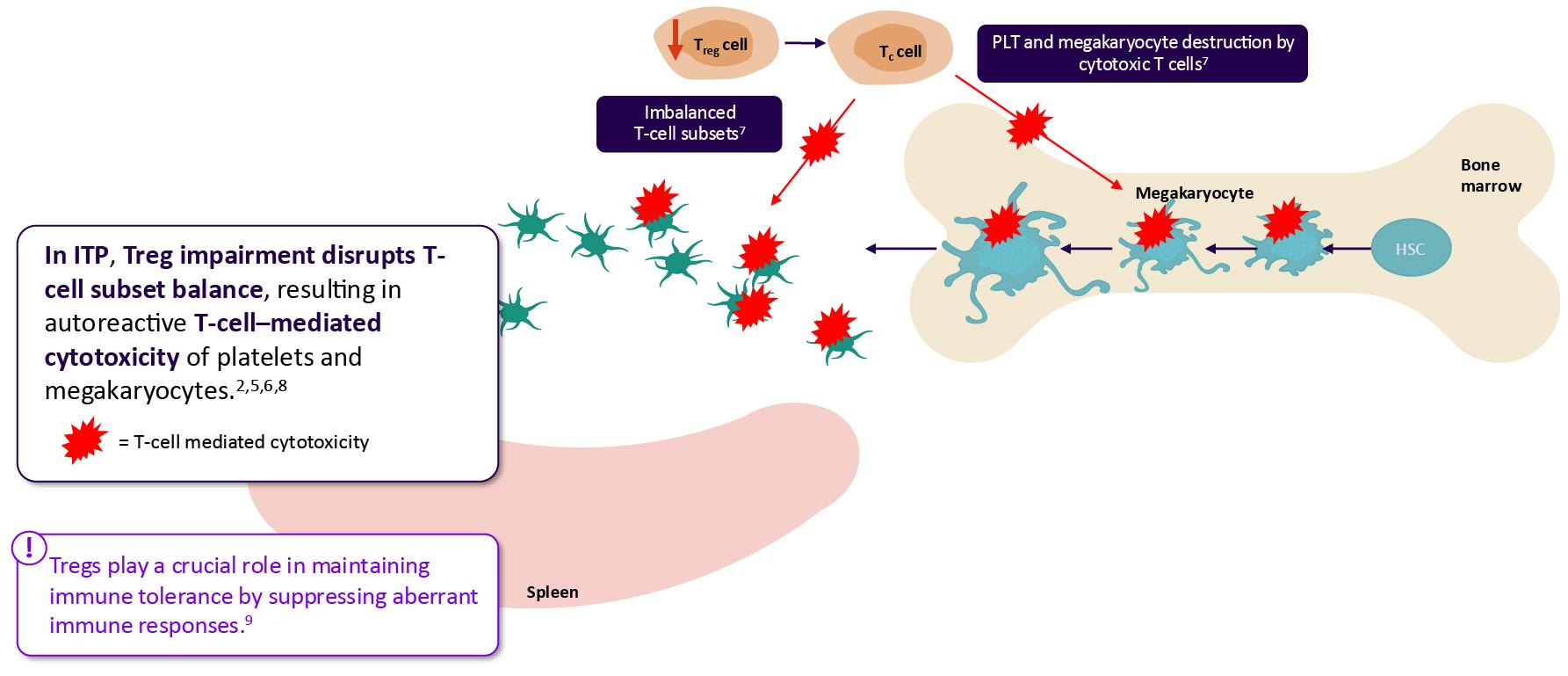
In healthy individuals, the regulatory interplay between innate and adaptive immunity allows for immune homeostasis.8,9,14
Tregs play a crucial role in maintaining immune tolerance by suppressing aberrant immune responses.8
.2025-12-19-16-14-44.jpg)
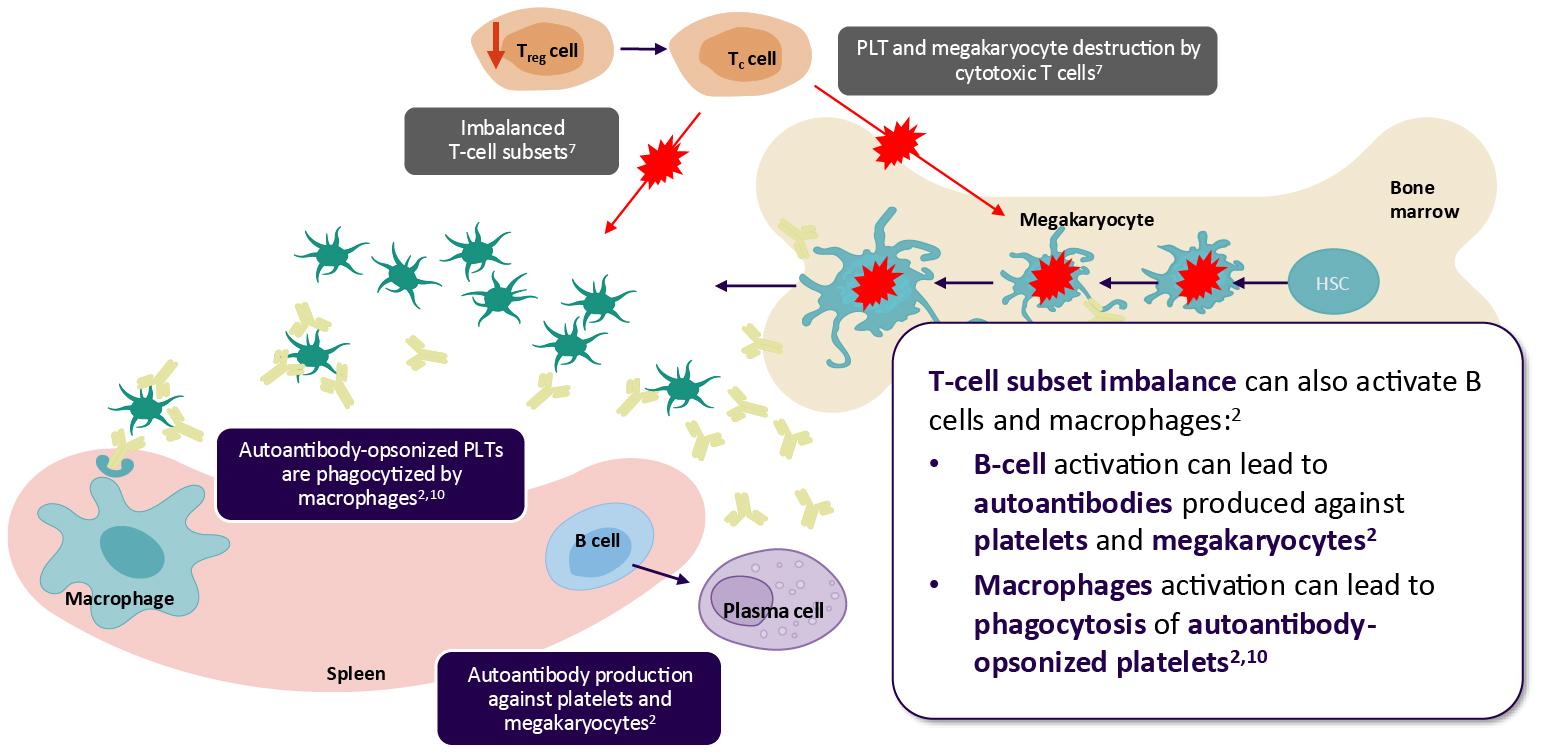
Th cells in the spleen activate B cells and macrophages, key players of immune response.2
Macrophages, primarily in the spleen, recognize and phagocytize autoantibody-opsonized platelets, leading to their rapid destruction.2,10
- This process activates macrophages to present platelet antigens and release pro-inflammatory cytokines, driving the inflammatory response in ITP
Regulation of immune response is impaired due to:
- Dysregulation of T cells leading to imbalance of proinflammatory factors10
- NLRP3 inflammasome activation driven
- Leading to a chronic pro-inflammatory state that further drives T-cell and B-cell dysfunction, contributes to platelet destruction, and amplifies the overall immune response in ITP.10
.2025-12-19-16-11-45.png)
Abbreviations:
HSC, hematopoietic stem cell; IL, interleukin; ITP, immune thrombocytopenia; NLRP3, nucleotide-binding domain leucine-rich repeat containing protein 3; PLT, platelet; Tc cell, cytotoxic T cell; Th cell, T helper cell; Treg, regulatory T cell.
*The fundamental etiology of ITP may arise from an environmental trigger occurring in a genetically predisposed patient, as well as potential expansion of innate lymphoid cells, but a definitive cause remains elusive.5
- Kuter DJ, et al. Ther Adv Hematol. 2023;14:20406207231205431.
- Martínez-Carballeira D, et al. Hematol Rep. 2024;16(2):204-219.
- Cooper N, Ghanima W. N Engl J Med. 2019;381(10):945-955.
- Wang R, et al. MedComm. 2024;5(10):e714.
- Tariq Z, et al. Front Biosci (Landmark Ed). 2024;29(10):342.
- Andreescu M. Front Hematol. 2023;2:1191178.
- Singh A, et al. J Clin Med. 2021;10(4):789.
- Bu S, et al. Front Immunol. 2025;16:1499014.
- Marshall JS, et al. Allergy Asthma Clin Immunol. 2018;14(Suppl 2):49.
- Audia S, et al. Hemasphere. 2021;5(6):e574.
- Wang S, et al. Thromb Res. 2021;199:1-9.
MAT-KW-2600104-V1-Mar-2026