Genetic disease2
AATD is an inherited disorder in which pathogenic variants in the SERPINA1 gene lead to low or undetectable levels of serum alpha-1 antitrypsin (AAT) protein.
Highly underdiagnosed3
70,000 to 100,000 individuals in the United States are estimated to be severely AAT deficient.a However, >90% of these cases are not diagnosed.
Spectrum of risk4,5
Genotype‑related differences in AAT levels can result in differing levels of risk for patients in developing lung disease.
Irreversible decline in lung function4,6-9
Insufficient levels of AAT increase the risk of lung disease such as COPD and emphysema. Behavioral, environmental, and pathophysiologic factors also influence this risk.
a<11 µM.10
AAT protects lung tissue from protease-induced damage11
AAT plays a key role in protecting the lungs by11:
- Inhibiting neutrophil elastase and dampening pro-inflammatory cytokine production
- Reducing cellular damage from reactive oxygen species (ROS)
- Supporting immunomodulatory pathways that help protect tissues from unchecked inflammatory activity
Genotypes and resultant AAT levels contribute to increased risk of irreversible lung disease4,6

- Genotype determines how much AAT protein a person produces4
- Below-normal AAT levels increase susceptibility to faster disease progression4,12
- Can lead to progressive lung damage, which may result in COPD and emphysema6
- Lung decline can be further accelerated by behavioral factors such as smoking, as well as environmental factors such as air pollution and dust7-9
- Those with certain genotypes may also experience liver disease and vasculitis11
Lower AAT levels are associated with higher risk of AATD-associated emphysema13
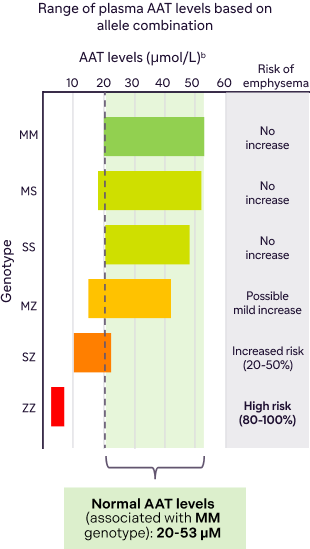
bAAT levels may also be measured in mg/dL.
Data from Mulkareddy V et al. Am J Med Sci. 2024;368(1):1-8.
Emphysema is the most common underlying cause of mortality in patients with severe deficiency of AAT14
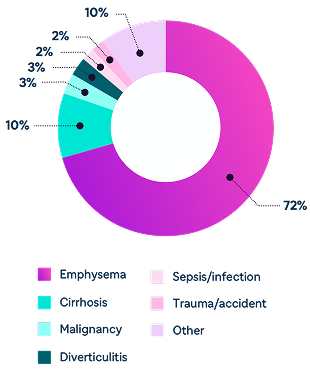
Underlying causes of death among 118 patients with severe deficiency of AAT (defined as serum level <11 µmol/L). Of the 118 patients, 13.7% were never-smokers and 86.3% were ever-smokers (National Heart, Lung, and Blood Institute Registry 1989-1992).14
Data from Stoller JK et al. Chest. 2005;127(4):1196-1204.
Clinical presentation of AATD overlaps with COPD, making diagnosis challenging15
Symptoms include4,16,17:
- Shortness of breath during daily activities
- Wheezing
- Decreased ability to exercise
- Excessive mucus production when coughing
Patients may also present with4,17:
- Asthma
- Bronchiectasis
- Bronchial hyperresponsiveness
ATS/ERS and GOLD guidelines recommend that all patients with COPD be tested for AATD1,4
Clinical presentation by itself is not enough to determine which patients with COPD may be living with AATD. Genetic and AAT protein level testing are definitive ways to achieve a diagnosis.12,15
Clinical practice guidance on testing for AATD (ATS/ERS, GOLD)1,4:
- All patients with a diagnosis of COPD
- Symptomatic individualsb
- First-degree relatives of patients diagnosed with AATD
bSymptoms that warrant testing for AATD include emphysema, asthma, unexplained chronic liver disease, necrotizing panniculitis, granulomatosis with polyangiitis, unexplained bronchiectasis, smoking exposure, and occupational exposure.4,12
AAT Protein Level Testing5,18,19 |
SERPINA1 Genetic Testing5,12 | |
WHY | Determine whether AAT protein deficiency is present and to assess severity | Confirm a diagnosis of AATD and determine a patient’s specific genotype |
WHAT | Quantitative measure of AAT serum levels | Identification of genetic alleles (M, S, Z, F, I, etc.) |
HOW | Whole blood, serum, dried blood spot sample Available methods include radial immunodiffusion, nephelometry, and latex-enhanced immunoturbidimetry | Whole blood, saliva, dried blood spot, cheek swab sample Detection via DNA sequencing or protease inhibitor (Pi) typing |
AATD testing is widely available (including sponsored testing at no charge).c
cThis is not an endorsement of any specific lab. Testing options can be found at https://www.ncbi.nlm.nih.gov/gtr/. Sanofi does not review or control the content of non-Sanofi websites. Consult each laboratory for a full range of options. Content is current at time of publication, and testing may not be available in all states; please call laboratory to confirm test availability, sample shipping information, and all other logistics. This listing does not constitute an endorsement by Sanofi.
AAT=alpha-1 antitrypsin; AATD=alpha-1 antitrypsin deficiency; ATS=American Thoracic Society; COPD=chronic obstructive pulmonary disease; ERS=European Respiratory Society; GOLD=Global Initiative for Chronic Obstructive Lung Disease; Pi=protease inhibitor; ROS=reactive oxygen species.
References: 1. Global Initiative for Chronic Obstructive Lung Disease. GOLD Report. Accessed February 3, 2026. https://goldcopd.org 2. Cazzola M et al. Eur Respir Rev. 2020;29(155):190073. 3. Lopez MA. Alpha-1 antitrypsin deficiency (AATD). Accessed March 25, 2026. https://www.rarediseaseadvisor.com/disease-info-pages/alpha-1-antitrypsin-deficiencyepidemiology-aatd/ 4. American Thoracic Society; European Respiratory Society. Am J Respir Crit Care Med. 2003;168(7):818-900. 5. Feitosa PHR et al. J Bras Pneumol. 2024;50(5):e20240235. 6. Meseeha M et al. Alpha-1 antitrypsin deficiency. In: StatPearls [Internet]. ncbi.nlm.nih.gov/books/NBK442030/ 7. Torres-Durán M et al. Orphanet J Rare Dis. 2018;13(1):114. 8. Wang T et al. Mol Med Rep. 2025;31(4):107. 9. Kokturk N et al. Respir Res. 2023;24(1):40. 10. Barjaktarevic I et al. BMC Pulm Med. 2021;21(1):99. 11. Mazzuca C et al. Front Immunol. 2024;15:1443297. 12. Sandhaus RA et al. Chronic Obstr Pulm Dis. 2016;3(3):668-682. 13. Mulkareddy V et al. Am J Med Sci. 2024;368(1):1-8. 14. Stoller JK et al. Chest. 2005;127(4):1196-1204. 15. Quinn M et al. Ther Clin Risk Manag. 2020;16:1243-1255. 16. Choate R et al. BMC Pulm Med. 2024;24(1):138. 17. Kalfopolous M et al. In: Borel F et al, eds. Methods in Molecular Biology. Humana Press; 2017:9-20. 18. Abboud RT et al. Appl Clin Genet. 2011;4:55-65. 19. Craig TJ et al. Allergy. 2018;73(11):2110-2121.
